
Greenslopes Private Hospital Patient Information
For patients requiring surgical treatment she operates at Greenslopes Private Hospital
Dr Sharon Kelly offers comprehensive care - ear, nose, and throat specialist care for a wide range surgical and medical disorders of the ears, nose and throat for both adults and children. Dr Kelly's specialities include Ear, Nose and throat surgery, Paediatric ENT, Otolaryngology, Head and Neck, Endoscopic management of stones in the submandibular ducts, Bone anchored hearing aids and management of snoring and sleep apnoea.
My healthcare rights
This is the second edition of the Australian Charter of Healthcare Rights.
These rights apply to all people in all places where health care is provided in Australia.
The Charter describes what you, or someone you care for, can expect when receiving health care.
I have a right to
Access
- Healthcare services and treatment that meets my needs
Safety
- Receive safe and high quality health care
- Be cared for in an environment that is safe
Respect
- Be treated as an individual, and with dignity and respect
- Have my culture, identity, beliefs and choices recognised and respected
Partnership
- Ask questions and be involved in open and honest communication
- Make decisions with my healthcare provider, to the extent that I choose and am able to
- Include the people that I want in planning and decision-making
Information
- Clear information about my condition, the possible benefits and risks of different tests and treatments, so I can give my informed consent
- Receive information about services, waiting times and costs
- Be given assistance, when I need it, to help me to understand and use health information
- Access my health information
- Be told if something has gone wrong during my health care, how it may affect me and what is being done to make care safe
Top Tips for Safe Health Care
What you need to know for yourself, your family or someone you care for.
1. Ask questions
You have the right to ask questions about your care.
2. Find good information
Not all information is reliable. Ask your doctor for guidance.
3. Understand the risks and benefits
Find out about your tests and treatments before they happen.
4. List all your medicines
Ask your doctor or pharmacist if you need more information about the medicines you are taking.
5. Confirm details of your operation beforehand
Ask to be told who will be doing your procedure and what will happen.
6. Ask about your care after leaving hospital
Ask for a written outline of your treatment and what should happen next.
7. Know your rights
You have a number of rights as a patient. Read your guide to find out more.
The Ramsay Rule for Patients
The Ramsay Rule is about keeping our patients safe by partnering with you and your family in care. Excellent care to our patients by focusing on your safety. The Ramsay Rule helps us to do this.
When to Activate the Ramsay Rule
Patients: When you are concerned about a change in your condition, feel that you may be getting worse, or that your concerns have not been followed up.
Families & Carers: You are concerned that your loved one is looking unwell, getting worse or their behaviour has changed.
You know yourself or your loved one best. So if you are worried, follow these three simple steps to act.
How to Activate the Ramsay Rule
Follow these steps to raise your concerns:
- Talk to the Nurse, Doctor or Midwife regarding your concerns; and if you are not satisfied that your concerns are being addressed,
- Ask to talk to the Nurse in Charge of the shift; and if you are still concerned then you or a family member can activate the Ramsay Rule.
- Activate the “Ramsay Rule” by ringing this phone number 3394 7111. A Ramsay Rule nurse or doctor will attend and conduct a review of the patient.
World class treatment is closer than you think
Caring for the community since 1942.
greenslopesprivate.com.au
About Greenslopes Private Hospital
Greenslopes Private Hospital is proud to be Australia’s leading private teaching hospital, owned and operated by Ramsay Health Care. Located on Brisbane’s south side just 5km from the CBD, we are dedicated to growing and investing in the best clinical teams to provide high quality treatment.
We offer around the clock care across all 32 specialty areas, from our 24/7 Emergency Centre and modern maternity ward to a large and expanded robotic surgical unit. Many of the experienced specialists work across both the public and private sectors.
Our commitment to quality and safety for our patients, staff and visitors is our highest priority. As part of Ramsay Health Care, we implement a number of programs and initiatives that support national accreditation and safety standards.
About Ramsay Health Care
Ramsay Health Care is a global health care company with a reputation for operating high quality services and delivering excellent patient care.
Established in Sydney, Australia in 1964 by Paul Ramsay AO, Ramsay Health Care has more than 50 years of experience delivering acute health care services. Today, the company delivers a range of acute and primary health care services across several countries, making it one of the largest and most diverse private healthcare companies in the world.
Ramsay facilities cater for a broad range of health care needs from primary care to highly complex surgery and rehabilitation. The company employs more than 77,000 staff and treats millions of patients every year in hospitals and clinics across Australia, France, the United Kingdom, Sweden, Norway, Denmark, Germany, Italy, Malaysia, Indonesia and Hong Kong.
History
A historical museum for Greenslopes Private Hospital has been established in one of the former “bunker” buildings originally used during World War Two, with only one still in existence.
The Bunker displays many old photos and newspaper clippings from the hospital’s past, dating back to the early days of the hospital. Visitors can enjoy the story of the hospital’s history through the audiovisual presentation which is shown in the bunker.
The Bunker is located on the lower lobby level and is open Monday to Friday, 9.00am – 5.00pm.
Gallipoli Medical Research Foundation
An initiative of Greenslopes Private Hospital, the Gallipoli Medical Research Foundation (GMRF) is a registered charity conducting life saving medical research on the hospital campus. Since being established in 2005, the Foundation has strived to enhance the health of the Australian community.
GMRF runs a number of major research programs across a range of specialty areas which support the clinical work being undertaken at the hospital.
In addition, GMRF supports a culture of research and education at the hospital by administering annual grants conducted by our nursing and allied health professionals. GMRF also provides grants for innovative interventions from the Cyril Gilbert Testimonial Fund.
Open Disclosure
Every patient has the right to be treated with care, consideration and dignity.
At this health service we respect this right, and we are committed to improving the safety and quality of the care we provide. We have a policy of open disclosure for when things do not go as planned with the care we provide. Open disclosure occurs when patients are unintentionally harmed during health care.
This leaflet aims to inform you, the patient, your family and carers about the open disclosure process.
More than 200,000 people are treated in Australian hospitals each day. Occasionally something does go wrong and patients may be harmed unintentionally.
Australian health service organisations are working to improve the way they handle things that do not go as expected.
Part of improving the way they manage these situations is by being open with you about what happened.
The process of communicating with you when things have not gone as expected is called open disclosure.
What is open disclosure?
Open disclosure is open discussion about incidents that caused harm to a patient.
If you have been harmed during your treatment, your doctor, nurse or other healthcare worker should inform you about what happened.
Health services encourage their staff, as well as patients and their family or carers, to identify and report issues so that patients are harmed less often and care can be improved.
When would open disclosure occur?
Most things that do not go to plan in health care are minor or are found before they affect you. For these situations, your doctor or nurse will talk with you about what went wrong in the same way they talk with you about other aspects of your care. They should talk with you as soon as they are aware of the incident.
If you are seriously harmed, you will be informed as soon as possible and an open disclosure meeting will be arranged.
If you think a serious incident has occurred which has not been acknowledged, tell your doctor, nurse or another member of staff.
What is the benefit of open disclosure?
Open disclosure is designed for when things do not go to plan in health care. It will:
- Inform you, and help you to understand what went wrong with your care
- Let you know what is being done to investigate what went wrong
- Explain the consequences of the incident for you and your care
- Assist you with any support you might need
- Let you know the steps the health service organisation will be taking to make care safer in the future
Is there any other information available?
There is a booklet for patients beginning an open disclosure process called Open disclosure of things that go wrong: a guide for patients.
You can get copies of it from the health service or from the Australian Commission on Safety and Quality in Health Care website.
Patient-centred care
Patient-centred health care is respectful of and responsive to the preferences, needs and values of patients and their families.
It is important for you to be actively involved in your care. There are several ways to be actively involved.
Communication about care
Everyday
During your hospital stay, staff are required to hand over clinical information to the employees who will be caring for you next. During this handover staff discuss your care with the healthcare team to ensure you are involved in your own care, giving you an opportunity to review and confirm information relevant to your health. The teams taking care of you will take this opportunity to review information relating to your health. Please feel free to contribute to this process.
If something is wrong
The hospital has a process in place that ensures an urgent review of patients whose health is deteriorating. If you are concerned, you will be reviewed by your treating medical team and nursing staff on a regular basis. If staff are concerned, they can activate the escalation of care process. The involvement of you, your family members and carers is also encouraged. Family members and carers know you well and spend more time with you, and they are ideally placed to identify if you or your relatives are concerned about the state of your health and require emergency assistance.
Privacy
Ramsay Health Care is bound by the Australian Privacy Principles under the Privacy Act 1988 (Cth) and governs how private health service providers handle personal information. We are committed to complying with all privacy requirements and ensuring that Ramsay Health Care collects, uses, discloses and stores your personal information responsibly.
The Privacy Statement sets out in brief how Ramsay Health Care will handle your personal information. To receive a copy of our full Privacy Policy, please visit our website www.ramsayhealth.com.au or ask for a copy of the Privacy Statement brochure.
Patient record
A patient record will be kept detailing your illness and treatment. This is confidential and access is limited to health professionals directly involved in your treatment. Your patient record will remain the property of the hospital and will not be divulged only with your written consent or where required by law. You may request access to your record at any time. The hospital has up to 14 days to respond to your request. Administration fees do apply. Please ask the Patient Records department to organise this.
Ward organisation
The ward areas are under the supervision of the Nurse Unit Manager during weekdays and a shift leader during evening, night and weekend shifts. Any problems that may occur during your stay should be raised with the nurse in charge.
Staff Identification
All staff wear name badges as a means of identification and internal security. The badge shows the staff member’s name and position.
Veteran Liaison Officer
Veteran patients are able to access the Veteran Liaison Officer who can act as a single point of contact for any issues or concerns that they may have. The Veteran Liaison Officer will refer the matter to the appropriate department if required. The Business Manager is the designated Veteran Liaison Officer for Greenslopes Private Hospital and can assist with enquiries.
Compliments / Complaints
We welcome compliments and feedback relating to your stay with us and we encourage all patients to complete a survey after they are discharged from hospital. The feedback we receive helps ensure we are meeting your expectations and to identify any areas needing improvement.
Ramsay Health Care continually seeks feedback on the experience of our patients. As part of this commitment, you may receive a survey asking about your visit to the hospital. We will use your feedback to make improvements and acknowledge staff who embody our commitment to patient care.
If you are concerned about your care or the hospital’s services whilst in hospital please ask for the Nurse Unit Manager on the ward. If you have been discharged please direct compliments or complaints to the Patient Liaison Officer. Feedback can be received by post, by telephone, by email using the hospital website, in person or through our survey system.
Contacts
It is always best to try to resolve your complaint with your local health service provider. If you have tried this and are still not satisfied, you can make a complaint to the Office of the Health Ombudsman.
Infection control
Hand hygiene is the single most important factor in reducing hospital acquired infections.
Our hands may look clean but many germs are invisible to our eyes. We can unknowingly transmit germs through contact with people, surfaces and our environment.
When should you clean your hands
Hand hygiene is a general term referring to the use of soap and water or a waterless alcohol based hand rub.
It is important to perform hand hygiene as you enter and leave a healthcare facility and also:
- Before and after visiting patients
- When your hands are visibly dirty
- After going to the toilet
- After handling or patting animals
- After handling soiled clothes or linen
- After coughing, sneezing, or blowing your nose
- After smoking
- Before eating
- Before, during and after preparing food
Standard Precautions
Hospital staff often wear gloves, aprons, masks or eye protection while caring for patients. This practice protects both patients and staff from transferring germs which can lead to infections.
Transmission Based Precautions
Sometimes patients have resistant germs that can easily spread to other people. To further prevent transmission based precautions may be used and a sign placed outside the patient’s room advising what precautions should be taken.
You may be asked to wear gowns, gloves and masks when visiting a patient under these precautions.
If you have questions
Do not be afraid to ask a healthcare worker if they have washed their hands.
If during your visit to our hospital you identify a risk or hazard that could cause harm or injury to another person, please inform the Department Manager or any of the staff on duty.
Working Together
Healthcare workers should always perform hand hygiene in front of you. If you did not see them do it, you have the right to remind them.
We can all play a major role in preventing the spread of infections to our family and friends.
For further information contact the Infection Control Department at Greenslopes Private Hospital or visit the website www.hha.org.au
Remember, infection prevention is everyone’s responsibility.
Emergency procedures
The hospital has well organised safety and emergency procedures in which each staff member has a specific role. In an emergency, remain in or by your bed until a staff member arrives to assist you.
Emergency procedures
The hospital has well organised safety and emergency procedures in which each staff member has a specific role in an emergency. Remain in or by your bed until a staff member arrives to assist you.
Smoke-free campus
Greenslopes Private Hospital is a smoke free campus.
From 1 September 2016, legislation in Queensland prohibits smoking within the hospital grounds and hospital boundary. There is also no smoking allowed within five metres of public transport waiting areas and taxi ranks. This applies to all persons including staff, doctors, volunteers, students, patients and visitors.
The laws are being enforced by government environmental health officers who will issue on the spot fines to individuals who ignore warnings and continue to smoke. We appreciate your support in promoting a healthy hospital community.
Violence/aggression
The hospital’s staff and patients need to work and be cared for in a safe environment, one that is free from violence and aggression. Any behaviour that threatens the safety of others will not be tolerated.
Going home
Once you have recovered from the acute phase of your surgery or illness, it is usual for you to continue your recovery at home. Hospital staff caring for you will keep you updated regarding your planned discharge date. If you foresee any difficulty returning home please discuss the issues with the staff caring for you as soon as possible, so that plans can be made for your return home.
Before your discharge the ward nurse will inform you when to make appointments for follow up, order medications to take home and make any other arrangements necessary for your after care.
On the day of your discharge it is expected that you will vacate your bed before 10.00am. If you are unable to leave by this time please make arrangements to fit this timeframe.
If your transport is delayed you may be asked to wait in the lounge area of the ward or in the Discharge Lounge.
If you have had a general anaesthetic or sedation within the past 24 hours you will need to be accompanied home. You should not drive a car, operate machinery or domestic appliances, conduct important business or sign legal documents following your anaesthetic.
Before you leave please ensure you have all your personal items including those that may have been placed in the hospital safe during your stay and follow up instructions.
Discharge planning
Discharge planning is an important part of any hospital admission. It plays an important role in ensuring a safe and smooth transition from hospital to home. This is achieved by making sure that appropriate clinical and community based support services are arranged prior to your discharge.
There are a number of people who can help plan your discharge
- You and your family or carer can alert us if your circumstances are such that you may need additional support after leaving hospital.
- Your treating doctor can help identify any special requirements you may have.
- Nursing and Allied Health staff may help identify services that you may require.
- Care Coordinators provide information and assist where possible to support you at home immediately after discharge.
- We want to make sure all issues that may affect your care after discharge are addressed before you leave hospital.
It is vital that any special needs following discharge are identified early so that the appropriate discharge arrangements can be made.
We encourage patients to discuss any issues with the healthcare team. These issues may be present if you:
- live alone
- are responsible for another person such as a frail partner or young children
- used community services prior to admission to hospital such as Meals on Wheels or community nurses
- require assistance to care for themselves such as showering
It is important that you consider all available options for care at home if your care needs have changed after your hospital stay. These services are not always readily available and not all patients are eligible for funded services.
Your Discharge Planning Checklist
These are the major factors to be considered in discharge planning. It is important for you to discuss these matters during your stay in hospital.
Accessing urgent services after discharge
Hospital staff may be able to refer directly to a Community Service Provider if there is an urgent need for support services which, if not met immediately, may place the patient at risk.
These services are available to:
- people aged 65 years and over
- Aboriginal and/or Torres Strait Islander people aged 50 years and over
The services that may be available include:
- nursing
- personal care
- meals
- transport
These services would be of a time limited duration (two weeks) with a longer term commitment only following referral and assessment.
Acceptance of the referral for urgent care by a Service Provider will be based on their capacity to take on the needs of clients awaiting services.
These services are subsidised by the Federal Government, and you will be required to make a co payment.
NDIS funding (existing)
You will need to discuss your care needs with your current NDIS Provider.
Under 65 years
Unfortunately, you are not eligible for services funded through the Commonwealth Home Support Programme and will need to access your services under a user pays model from a service provider.
Existing Community Services and Home Care Packages
If you were receiving Community Services prior to your hospital admission, it is important that you let the service provider know you are being or have been admitted to hospital so your services can be placed on hold.
When you are nearing discharge, please discuss your services with your Nurse, so we can ensure your services recommence in a timely manner after your discharge.
Other support services available you may be able to arrange when at home:
If you are an older person and are going to need help to stay at home and be more independent in the future, you may benefit from additional services available through the Commonwealth Home Support Programme.
Patients or their Carers need to commence this process. My Aged Care is the entry point to access these services.
Commonwealth Home Support Programme (CHSP)
What services are available under CHSP?
- personal care such as help showering and dressing
- shopping assistance
- transport
- home help such as cleaning
- nursing including wound care and medication assistance
- allied health services such as physiotherapy and occupational therapy
- meals
- modifications to your home such as rails and ramps
Who pays for the services?
The Australian Government contributes to the cost of aged care services.
How much you pay will depend on:
- your financial situation
- the number and types of services you receive
- the service provider
My Aged Care will:
- organise a face to face assessment by the Regional Assessment Service (usually within three weeks)
- provide details around costs
- help organise the right services for you
How to access services
- Call My Aged Care on 1800 200 422
- Access online at www.myagedcare.gov.au
If you are a veteran or war widow/er
You may also be eligible for Department of Veterans’ Affairs services or programs.
Looking After Yourself in Hospital
Falls Prevention
Our staff are here to assist you and help you.
Greenslopes Private Hospital utilises a falls prevention process to maintain the safety of our patients.
Did you know that many unplanned incidents in hospital are related to falling? While only some falls cause serious injury, they can affect a patient’s confidence and mobility, making it harder to stay independent.
Most falls in hospital happen when people are moving around, including
- Getting out of bed
- Walking, especially to the toilet
- In bathrooms and toilets
- Bending over reaching for personal items
Safety for our patients at risk of falls
Patients can become more susceptible to falling during their stay in hospital. Some of the reasons for this include:
- Being unwell
- Unfamiliar surroundings
- Medications prescribed or changed
- Surgery and effects of anaesthetics
- Poor balance
- Unsafe footwear
- Obstacles in the environment
- Hurrying to the toilet
- Change in independence
- Confusion
To our patients
Precautions you can take to decrease your risk of falling
- Familiarise yourself with your surroundings
- If advised by a nurse, always ring the call bell for assistance or supervision to mobilise around the ward
- It is important to remain active even in hospital. If recommended, take a slow walk once or twice a day
- When walking, take your time when turning around
- Notify staff if you use a walking aid. If you have your own walking aid please arrange for it to be brought to hospital
- Wear closed, non slip slippers, shoes or socks with grip soles. Do not walk in socks without grip
- Make sure loose robes are wrapped around snugly and loose belts and ties are fastened securely
- Make sure hems are not too long
- Always get out of bed slowly. Sit on the side of the bed for a few moments before standing
- Move your feet up and down to get the blood pumping
- Do not grab onto anything for support unless you know it is fixed and sturdy
- If you have glasses, wear the distance ones when mobilising
- Ensure your call bell is always close at hand
- Notify staff if you require a night light. At night turn the light on before mobilising
- Notify staff if you slip, trip or fall even if you are not hurt
- Let staff know if you feel unwell or unsteady on your feet
- Keep fluid levels up and ensure healthy eating
- Report spills immediately
Bathroom safety tips
- A staff member may need to stay with you for safety
- Sit down to shower and use the rails to get up off the chair or toilet
- Remain seated in the bathroom and use the call bell if you need help moving around
To our visiting family and friends
Precautions you can take to decrease a patient’s risk of falling
- Arrange for patient’s own walking aids to be brought into hospital
- The call bell and other important belongings such as glasses and books should be placed within easy reach
- Provide non slip shoes that fit well
- Report any spills, trips or falls immediately
Pressure Injury Prevention
What is a Pressure Injury?
A pressure injury (also known as pressure ulcer, pressure sore or bed sore) is an area of skin that has been damaged due to unrelieved pressure.
Where can pressure injuries be found on the body?
Pressure injuries are most commonly found over bony areas such as hips, spine and heels. They can also occur on other parts of the body depending on a person's position for long periods of time.
Let your Nurse know if you have any concerns regarding pressure or pain.
How can we work together to help reduce your risk of developing a pressure injury?
We are here to help by:
- Completing a full skin and pressure injury risk assessment when you come into hospital and regularly during your stay
- Tailoring a plan with you to prevent and manage any risks you may have of developing a pressure injury
This plan may include various strategies depending on your specific needs such as applying protective dressings, using pressure relieving equipment or assisting you to change position regularly.
Prevention of Blood Clots in Hospital – Blood Clots: DVTs and PEs
If a blood clot forms in your leg (Deep Vein Thrombosis or DVT), it can affect blood flow and cause swelling or pain. In some cases, it may lead to permanent damage to your leg.
Fragments of these blood clots can break off and then travel through your veins to your lungs and block blood flow. This is called a Pulmonary Embolus or PE. This is a serious condition which can be fatal.
When you are admitted to hospital you are at higher risk of developing a blood clot. Early detection and prevention are important to reduce the risk of harm. To determine your level of risk an assessment will be completed by your healthcare team.
The assessment may consider:
- Your age
- The reason you are in hospital
- Any other health problems you have or have had in the past
Risk factors for Blood Clots
- Smoking
- Age over 60 years
- Severe lung disease
- Having had a blood clot in the past
- Reduced mobility
- Surgery or trauma
- Cancer or cancer treatment
- Obesity
Your treating doctor will discuss treatment options with you. Treatment may include:
- Wearing compression stockings
- Using compression pumps on your lower legs or feet
- Taking tablets or injections to help prevent a blood clot
- Gently exercising your feet and legs in bed
- Getting out of bed and walking as soon as possible
Some of these treatments are not suitable for some people. If you are at high risk, your health care team may adjust your treatment plan. Ask your doctor what treatments they recommend for you.
What can you do to help?
You can help your health care team reduce the risk of a blood clot forming.
While in hospital
- Make sure you take any tablets or injections your doctor has prescribed to reduce your risk.
- Keep your compression stockings on and do not let them roll down. Please let your nurse know if they become uncomfortable.
- Avoid sitting or lying in bed for long periods.
- Walk as often as your doctor advises.
Before you leave hospital
Ask your doctor about what you should do at home to prevent a blood clot:
- How long to wear your compression stockings
- Do you need blood thinning medication at home?
- What physical activity you need to do
- Should you avoid alcohol?
- Other things you can do to reduce your risk of a clot
Prevention at home
- Avoid sitting for long periods
- When sitting, do your leg exercises
- Drink plenty of fluids
- If travelling long distances, make frequent stops to get out and walk around
Symptoms to be aware of
- Pain or tenderness and a warm feeling in your legs
- Swelling of the lower leg, ankle and foot
- Sharp pain in your lungs or chest
- Difficulty breathing
If you experience any of these symptoms after you have left hospital, seek immediate emergency care by attending your closest hospital emergency centre. You should also notify your doctor.
Nutrition for recovery
Good nutrition plays a very important role in your recovery from illness or surgery. Your protein and energy needs increase during recovery as the body works to rebuild and repair body tissue. This means you may need to consume more food and nutrients to meet your body’s protein and energy requirements.
Sometimes a poor appetite or feeling unwell can make this difficult to achieve. The following strategies may help you increase your intake of nutritious foods while in hospital.
Foods to increase protein and energy intake
Protein rich foods include meat, ham, chicken, fish, eggs, nuts, baked beans, dairy foods such as milk, yoghurt and cheese, as well as soy milk. These foods are also high in energy and can help support your recovery.
Nutrition for recovery meal suggestions
| Meal | Menu Items |
|---|---|
| Breakfast | Yoghurt, milk, porridge with milk, eggs, baked beans |
| Lunch and Dinner | Main course, dairy desserts such as custard, crème caramel, ice cream, yoghurt and creamed rice |
| Between meals | Milk or milk drinks, cheese, yoghurt |
Other ideas to assist you in increasing your intake
- Eat small meals more often throughout the day
- Choose foods that are high in protein and energy
- Drink nutritious beverages such as milk or smoothies
- Ask staff if you need assistance with meal options
Nutrition for recovery
Weight is taken on admission to hospital and weekly thereafter. This can be used as a measure of how well your nutritional needs are being met. You should aim to avoid weight loss in hospital, even if you are overweight. Weight loss due to illness can delay recovery. Overweight issues can be addressed once you have recovered from your hospital stay.
If you are using all of the above strategies and your weight is still decreasing, ask your nurse or doctor for advice. Nutritional supplementation and other strategies may be required.
Caring for your IV cannula / drip
What is an IV / drip and why do I need it?
An IV (intravenous) drip is a small, soft plastic tube (cannula) inserted into a vein, usually in your hand or arm. It allows fluids, blood transfusions or medications such as antibiotics to be given directly into your bloodstream.
How is your IV cannula put in?
Your doctor, nurse or midwife will:
- Verify your name and check for allergies, explain the procedure and obtain verbal consent
- Wash their hands and wear gloves
- Clean your skin with an antiseptic and use sterile equipment
- Place the IV into a vein using a fine needle, which is removed after the plastic tube (cannula) is in place
- Cover the IV insertion site with a sterile dressing and write the date on the dressing
Is having your IV cannula inserted painful?
You may feel a brief sting as the needle goes in, but once the cannula is in place this should pass. The cannula is usually inserted in the inside of your elbow or hand. If you experience ongoing pain after the IV is inserted please notify your nurse.
Can the cannula fall out?
The IV cannula is secured with a see through dressing and is taped in place to prevent it falling out. Please let staff know if the dressing becomes loose or painful.
Are there any risks of having an IV?
- There is a small risk of infection with any procedure that punctures the skin. As an IV sits directly in your vein there is a higher risk of infection.
- Difficult or unsuccessful attempts to insert an IV can cause bruising and the cannula may cause irritation.
- Sometimes the IV cannula may become blocked by blood and may need to be removed.
- The cannula should be replaced every 72 hours if still required.
Important: Let staff know straight away if you notice any redness, swelling, skin irritation, heat, bleeding or if the area feels hot, cold or shivery.
A nurse should check your cannula each shift. Please ask your Doctor or Nurse each day if you still need the IV.
How can you help in the care of your IV?
- Try not to touch the IV site or pull or knock the tubing
- Try to keep the dressing clean and dry
- It is ok to remind staff to clean their hands before touching your IV
- Your IV should not be disconnected from the fluid bag when you shower or are getting dressed
- Wash your hands after going to the toilet
- The IV should be removed before you are discharged from hospital
- Your IV and dressing should look similar to the picture shown by your nurse
Working Together
Healthcare workers should always perform hand hygiene in front of you. If you did not see them do this, you have the right to remind them.
We can all play a major role in preventing the spread of infections to our family and friends.
Patient room
Call button
Should you require assistance at any time, alert the nursing staff using the nurse call button located in your room. This allows you to buzz for assistance and speak directly to staff at the ward nurses’ station. The light will illuminate at the nurses station. After attending to your needs the nurses will cancel the call.
Catering
Our Catering Department prepares a variety of high quality, fresh meals to suit a range of dietary requirements. The catering team will provide you with information on the menu each day and offer you a range of selections to choose from.
Electrical items
Whilst we wish to support your stay in hospital and make it as pleasant as possible, we have an obligation to maintain a safe environment. As we cannot ensure the safety of your own personal electrical items, we request that you keep these items at home.
Patient supplied medical devices are only permissible if they have been tested by our Biomedical Department to ensure they meet hospital standards. Electrical heating pads are not permissible due to the inherent fire hazards associated with these products.
Telephones
You can make and receive free local calls from the telephone by your bed by dialling 0 and then the number you wish to call.
STD and ISD telephone calls cannot be made without the purchase of a telephone card, which can be obtained from the hospital kiosk or Main Reception.
People may phone you directly by dialling 3329 followed by the extension number provided on your phone. Alternatively they may phone (07) 3394 7111 (Hospital Switchboard) and ask to be transferred to your bedside telephone between 7.00am and 10.00pm.
If you do not want calls to be transferred through to you please only give your direct line to those friends or relatives you wish to contact you. Please advise a staff member to notify Switchboard not to transfer calls to you.
The use of mobile phones is restricted within the hospital environment due to risks of interference with medical equipment. Visitors and patients are asked to turn off their mobile phones when entering a patient care area.
Full list of Channels available
| No. | Channel Name | No. | Channel Name | No. | Channel Name |
|---|---|---|---|---|---|
| 1 | ONE | 30 | SBS HD | 203 | SBS Arabic 24 |
| 2 | ABC | 31 | SBS Viceland HD | 204 | SBS PopDesi |
| 3 | SBS ONE | 32 | SBS World Movies | 205 | SBS Chill |
| 7 | 7 Brisbane | 33 | Food Network | 301 | SBS PopAsia |
| 9 | Channel 9 Brisbane | 34 | NITV | 302 | SBS Radio 2 |
| 10 | TEN Digital | 36 | SBS Arabic 24 | 303 | SBS Radio 3 |
| 11 | Ten Peach | 73 | 7 Mate Brisbane | 304 | SBS Arabic 24 |
| 12 | Ten Bold | 74 | 7 Mate HD | 305 | SBS PopDesi |
| 13 | Ten Share | 75 | Openshop | 306 | SBS Chill |
| 15 | Ten HD | 76 | 7flix Brisbane | 307 | SBS PopAsia |
| 16 | TVSN | 78 | RACING.COM | 401 | Welcome / Information |
| 17 | Spree TV | 90 | 9 HD Brisbane | 402 | Fox Classics |
| 20 | ABC HD | 91 | Channel 9 Brisbane | 403 | Fox Lifestyle |
| 21 | ABC | 92 | 9 Gem | 404 | Fox 8 |
| 22 | ABC2 / Kids | 93 | 9 Go | 405 | Fox Footy |
| 23 | ABC ME | 94 | 9 Life | 406 | Fox League |
| 24 | ABC News 24 | 95 | 9 GEM HD Brisbane | 407 | Fox Sport 503 |
| 25 | ABC Brisbane | 96 | 9 Rush Brisbane | 408 | Fox Cricket |
| 26 | ABC RN | 97 | Extra | 409 | Fox Crime |
| 27 | ABC Classic | 99 | 9 Go | 410 | Fox Funny |
| 28 | Triple J | 200 | Double J | 411 | Nickelodeon |
| 29 | Triple J Unearthed | 201 | ABC Jazz | 412 | Fox Arena |
Valuables
The hospital will not accept liability for loss of valuables or personal belongings and patients will be asked to sign a disclaimer on admission. Patients throughout the hospital have access to a safe in most rooms which operate with a unique four digit pin number. Further instructions are available in patient rooms next to the safe. After admission, please use the in room safe for valuables where possible.
Due to fire and security risks we cannot provide safekeeping for larger items including wallets and laptops.
Patient & visitor services
ATM facility
An Automated Teller Machine (ATM) is located on the Lobby Level near the coffee shop.
Chaplaincy and pastoral support services
Chaplaincy and Pastoral Support Services offer patients, staff, family and friends emotional and spiritual support. This service is available to people of all faiths or those with no religious affiliation. A chaplain can provide support when a person feels lonely, distressed, anxious or simply needs someone to listen.
Coffee shop
Hudsons Coffee is located on the Lobby Level of the hospital and is open 7 days a week, between 6.00am and 7.30am and 6.00pm Saturday and Sunday.
Hudsons Coffee also has an outlet on the Ground Floor of the Administration Building in the Greenslopes Outpatients Department which is open between 8.00am and 3.00pm Monday to Friday. Hours may vary.
Free shuttle bus service – the GPH Express
The GPH Express operates between the Greenslopes Translink Busway Station and the main entrance of the hospital Monday to Friday (excluding public holidays), between 6.00am and 6.00pm (approximately every 15 minutes).
For information on local transport that connects with the Greenslopes Busway and phone 13 12 30 or visit the Translink website.
For further information regarding the GPH Express please call: 07 3394 7033
Free RSL courtesy bus services
A free bus service is operated from Monday to Friday by the Kedron-Wavell RSL Sub Branch. It provides transport for veterans, carers and relatives to Greenslopes Private Hospital. For schedules and bookings please contact the RSL.
Hairdresser
An onsite hairdressing service is available for patients. Please advise the ward secretary who will organise an appointment. Charges apply.
Internet access
How to connect
- Ensure your wireless enabled laptop or mobile device is turned on and has its wireless signal switched on.
- Go to the available Wireless Network Connection List as displayed on your laptop or mobile device.
- Click on WiFi@Ramsay and then click on the Connect button. Your Internet Browser will automatically open and you will be prompted with the “Welcome to Ramsay WiFi” page.
- Select the appropriate option: Patient or Guest. The option that you select will display a second page where you can register for WiFi as shown in the windows below.
- Enter your details as required. NB: Your MRN is created on admission and is usually on your wristband. Please enter all 10 characters of the MRN.
- Review the Usage Policy and Terms and Conditions and tick the box to accept the terms of use. Accepting the terms and conditions is necessary if you want to use the WiFi facility.
- Click on the LOGIN button to proceed to the internet.
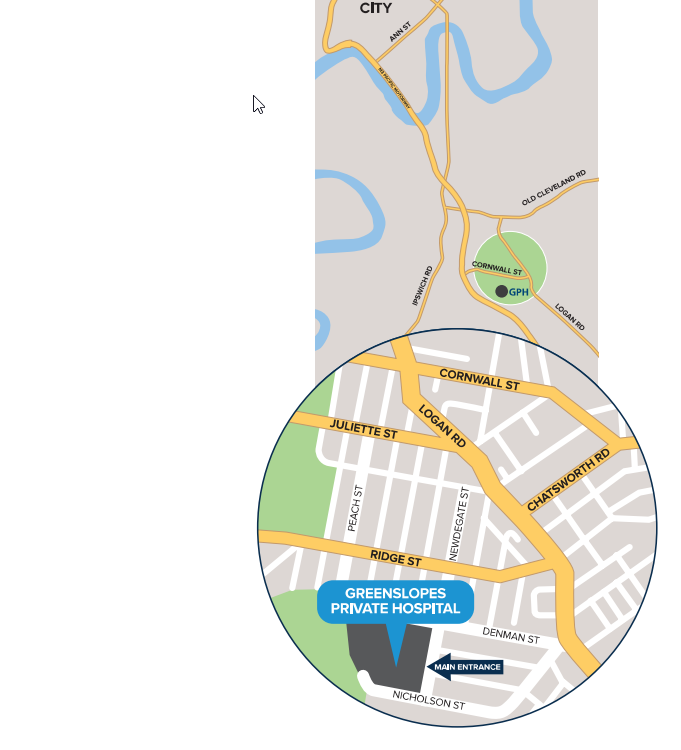
Greenslopes Private Hospital
Newdegate St, Greenslopes QLD 4120
For more information, please download the patient information booklet.